Elsa Reallon,a,† Anne-Laure Yailian,a,b,†,* Chloé Marchand,a,c Samira Filali,a,c Camille Merienne,a,c Christine Pivot,a Carole Pailleta and Fabrice Pirota,c
aService Pharmaceutique, Groupement Hospitalier Centre, Hôpital Edouard Herriot, Place d’Arsonval, F-69437 Lyon Cedex 03, France. *Corresponding author: [email protected]
bUniversité Claude Bernard Lyon 1, EA 4129 P2S Parcours Santé Systémique, 7-11 rue Guilllaume Paradin, 69008 Lyon, France
cLaboratoire de Recherche et Développement de Pharmacie Galénique Industrielle, UMR 5305, Plateforme Fripharm, Faculté de Pharmacie, Université Claude Bernard Lyon 1, 8, avenue Rockefeller, F-69373 Lyon Cedex 08, France
†These authors have contributed equally to this work
DOI: https://doi.org/10.1255/sew.2021.a27
© 2021 The Author
Published under a Creative Commons BY-NC-ND licence
Confusion regarding the identification of medicines by patients, physicians and pharmacists is a major concern. Here, we detail the successful identification of unlabelled medicine from a new tool named Medicine Identification New Database (MIND) implemented in our hospital pharmacy. Web tools (drugs.com, WebMD, Google Lens) and MIND were used for identification of an unlabelled unitary (single tablet/capsule) medicine returned from the care unit. MIND combines three modules including organoleptic (form, shape, colour), physical (dimensions, mass) and attenuated total reflectance-Fourier transform infrared spectra of oral medicines. While the web tools failed to identify unlabelled the unitary medicine properly, MIND discriminated the pharmaceutical product and confirmed, from infrared spectroscopy, the real identity of the medication and major excipients. The simplicity of the approach combined with the accuracy of the physical and spectral characterisation confirmed the potential of MIND as suitable tool for quick, simple and accurate identification of unlabelled medication in hospital pharmacies.
Introduction
From prescribing a medication to administrating it to a patient, the journey of medicines is marked out by many stages, in an intricate network which must guarantee the secure handling of the medications. As an essential part of a medicine management system, hospital pharmacies ensure that an appropriate system is implemented for the handling of stock medicines from their receipt from external suppliers to their dispensing to patients. As matter of fact, the supply of medicines from a hospital pharmacy is a complex process, since a medicine may be needed as a unitary (single tablet/capsule) or multi-dose. The latter first involves an unpacking step from the original packaging, then a subsequent unitary repackaging with the potential for incomplete medication labelling [i.e. with international non-proprietary name (INN), dose, expiry date and batch number] and confusion1 between different drugs. Therefore, to ensure the safety of these intermediate steps, quality control allowing a fast and reliable identification of the unitary medicine is desirable before ward dispensation to prevent harmful errors during administration to patients. In order to improve the identification of oral medicines, a dedicated database named MIND (Medicine Identification New Database) was developed by our hospital pharmacy. MIND includes three modules running with (i) commercial information [manufacturer, CAS registry number and active pharmaceutical ingredient (API)], (ii) organoleptic properties (type, shape, colour, size, weight) and (iii) an attenuated total reflectance-Fourier transform infrared (ATR/FT-IR) spectrum of oral medicines. The ATR/FT-IR module, which contains more than 500 entries, was initially built-in house then transferred to S.T.Japan-Europe GmbH (Pharmaceutical Tablets and Capsules Database L30030). Here, we describe a successful application of MIND for the identification of a returned and undetermined unitary medicine from an intensive care unit in which 15,000 dispensations of medicines per year are performed.
Methods
An unidentified unitary medicine (orange/clear capsule filled with white pellets) without mandatory information (INN, dose, expiry date and batch number) was returned to the hospital pharmacy for proper identification. Preliminary identification using free online databases (drugs.com, WebMD and Google Lens) was conducted by considering the colour and the shape of the capsule. Complementarily, the mass and the size of the capsule were determined, then input to MIND for an initial screening for potential medicines. Furthermore, to refine the accuracy of identification, an infrared spectrum of the capsule content was measured after capsule opening and pellet crushing. The infrared spectrum was recorded using an ATR/FT-IR spectrometer (3800–400 cm1, 10 cm optical path, 32 scans with spectral resolution of 4 cm1, Nicolet® iS 50 FT-IR spectrometer, Thermo Fisher Scientific).2,3 The ATR/FT-IR spectrum obtained was compared to the MIND ATR/FT-IR spectrum module database. Finally, a multi-component deconvolution of the initial spectrum was carried out to identify up to four individual components of the unknown crushed pellets.
Results
According to colour and shape description, drugs.com and WebMD websites failed to identify the unknown medicine and suggested more than 150 potential results, while Google Lens found 28 results after uploading a picture of the capsule. In running MIND, 4 results were found using colour and shape criteria (50 results with shape only; 27 with colour only). Adding the mass (154.4 mg) and the size (14.3 × 5.7 mm) of the capsule, MIND indicated that the unknown medicine was urapidil, 30 mg (Stragen Pharma SA, Plan-les-Ouates, Switzerland). This was finally confirmed by ATR/FT-IR analysis with 96 % similarity. Furthermore, the multi-component analysis of the crushed pellet indicated that saccharose was the major excipient. Figure 1 shows the assumed geometry of the hard capsule pellet (according to its composition and its active ingredient release profile) and the organoleptic, physical and spectral MIND characterisation. ATR/FT-IR spectra of 30 mg and 60 mg urapidil crushed pellets showed saccharose as a likely core excipient. Major saccharose contribution was shown in the D1 (3600–1750 cm–1) and D2 (1500–400 cm–1) parts of the ATR/FT-IR spectra of urapidil loaded pellets, while the ABC part of the spectra was attributed to the infrared contribution of the outer (A) and inner (B) layer components as well as the drug layer (C).
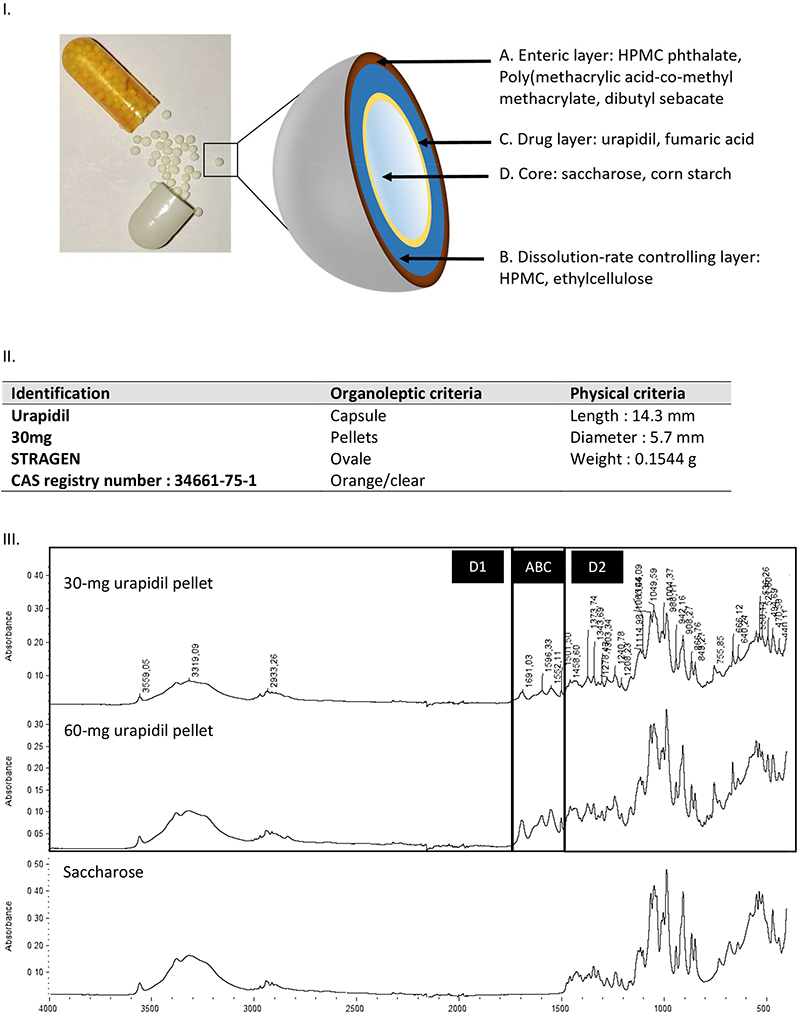
Figure 1. I) Photo of a capsule and interpretation of the geometry of urapidil pellets, assuming the presence of outer enteric and inner dissolution-rate-controlling layers surrounding the urapidil layer and core of the pellet. II) Identification made by MIND from organoleptic and physical criteria. III) ATR/FT-IR spectra of 30 mg and 60 mg urapidil crushed pellets and saccharose as the core excipient. Major saccharose contributions are shown in the D1 (3600–1750 cm–1) and D2 (1500–400 cm–1) parts of the ATR/FT-IR spectra of urapidil loaded pellets, while the ABC part is attributed to the contribution from the outer (A) and inner (B) layer components, as well as the drug layer (C).
Discussion
This short report highlights the effective screening strategy using a three-module (organoleptic, physical and mid-infrared spectral) database in a combined approach for the identification of medicines throughout the journey of both pharmaceutical product and patient in hospital. MIND consists of more than 500 entries from different types of medicines acquired and stored in the database. This tool enables quick and simple identification of medicines, e.g. (i) after medication removal from the original blister packaging followed by filling of unlabelled medicine into individual bags before dispensing, (ii) brought by the patient himself or relatives, (iii) mixed up with another medicines in care units before administration, (iv) counterfeit or (v) questioned for their physicochemical integrity and stability after long-storage in various conditions of temperature and humidity. A further useful application of MIND might be in the training of pharmacy technicians preparing individual pill organisers for patients.4 No sample preparation (allowing the medicine integrity to be maintained) or only straightforward crushing of medicines are required to analyse medicine by ATR/FT-IR spectroscopy5 enabling, in conjunction with organoleptic and physical properties, the discrimination of medications, the quality of pharmaceutical products and the characterisation of components from the mid-infrared spectra.6 Reproducibility (>93 %) and repeatability (>95 %) of spectral recognition were assessed from different solid oral forms belonging to one or more lots against respective reference spectra. By varying the resolution and the scan number, ATR/FT-IR spectroscopy ensured discrimination between medicines containing the same API or excipients.
Besides ATR/FT-IR, near infrared (NIR) and Raman spectroscopy were successfully used as sensitive and fast analytical techniques for the authentication and quality analysis of pharmaceutical products.7 Interestingly, portable NIR spectrometers offer great potential for rapid qualitative analyses, greatly improving the throughput of the control procedures.8 According to the field of application and the sample properties, NIR and ATR/FT-IR spectroscopy have different advantages and disadvantages. Thus, NIR penetrates deeply into materials and can be used for quality control measurements of pills and powders, but the absorption bands are relatively weak and not clearly delineated because they occur in the overtones of the fundamental bands in the mid-infrared region. Even though many compounds are not Raman active, Raman spectroscopy presents the major advantage of having no or minimal interference from water, and samples can be analysed through glass or polymer packaging.
Although pharmaceutical product serialisation improves medication safety by placing obligatory features on the outer packaging of medicines (i.e. a unique identifier and an anti-tampering device),9 the identification of each individual tablet (drug name, dose, batch number and expiry date) in blister packaging cannot be directly guaranteed. So, serialisation guarantees identification of the medicine throughout the pharmaceutical supply chain as far as its dispensing, but cannot be used after removal of the product from its initial packaging and subsequent distribution. Recent studies have reported that incorrect identification of look-alike tablets or pills figures prominently amongst fears surrounding medication errors,10 while “sound-alike look-alike” medication confusions harm as many as a quarter of a million of Americans annually.11
The development of MIND into a smartphone application coupled with a portable spectrometer may be useful for a variety of health professionals wishing to identify medicines. The content of the MIND databases requires continuous updating to include new medicines, and to modify existing medicines for any changes of the solid oral form.
Conclusion
The identification of medicine throughout the pharmaceutical supply chain and the hospital patient’s journey is a challenge which may be overcome by using screening pharmaceutical databases consisting of organoleptic, physical and spectral information.
Competing interests
The ATR/FT-IR spectrum module of MIND was sold by Hospices Civils de Lyon as an individual entity to S.T.Japan-Europe GmbH.
References
- J.L. Cina, T.K. Gandhi, W. Churchill, J. Fanikos, M. McCrea, P. Mitton, J.M. Rothschild, E. Featherstone, C. Keohane, D.W. Bates and E.G. Poon, “How many hospital pharmacy medication dispensing errors go undetected?”, Joint Comm. J. Qual. Patient Saf. 32(2), 73–80 (2006). https://doi.org/10.1016/S1553-7250(06)32010-7
- S. Filali, C. Bergamelli, M. Lamine Tall, D. Salmon, D. Laleye, C. Dhelens, E. Diouf, C. Pivot and F. Pirot, “Formulation, stability testing, and analytical characterization of melatonin-based preparation for clinical trial”, J. Pharm. Anal. 7(4), 237–243 (2017). https://doi.org/10.1016/j.jpha.2017.04.001
- C. Merienne, C. Marchand, S. Filali, D. Salmon, C. Pivot and F. Pirot, “Measurement, analysis and prediction of amoxicillin oral dose stability from integrated molecular description approach and accelerated predictive stability (APS)”, Pharm. Tech. Hosp. Pharmacy 5(1), 20200009 (2020). https://doi.org/10.1515/pthp-2020-0009
- A. Gadri, R. Pichon and G.L. Zelger, “A qualitative systemic analysis of drug dispensing in Swiss hospital wards”, Pharm. World Sci. 30(4), 343–352 (2008). https://doi.org/10.1007/s11096-007-9184-1
- D. Custers, T. Cauwenbergh, J.L. Bothy, P. Courselle, J.O. De Beer, S. Apers and E. Deconinck, “ATR-FTIR spectroscopy and chemometrics: An interesting tool to discriminate and characterize counterfeit medicines”, J. Pharm. Biomed. Anal. 112, 181–189 (2015). https://doi.org/10.1016/j.jpba.2014.11.007
- M.M. Said, S. Gibbons, A. Moffat and M. Zloh, “Use of near infrared spectroscopy and spectral databases to assess the quality of pharmaceutical products and aid characterization of unknown components”, J. Near Infrared Spectrosc. 27(5), 379–390 (2019). https://doi.org/10.1177/0967033519866009
- S. Lohumi, S. Lee, H. Lee and B.-K. Cho, “A review of vibrational spectroscopic techniques for the detection of food authenticity and adulteration”, Trends Food Sci. Technol. 46(1), 85–98 (2015). https://doi.org/10.1016/j.tifs.2015.08.003
- K.B. Bec´, J. Grabska and C.W. Huck, “Principles and applications of miniaturized near-infrared (NIR) spectrometers”, Chem. Eur. J. 27(5), 1514–1532 (2021). https://doi.org/10.1002/chem.202002838
- D. Ilko, C. Steiger, R. Keller, U. Holzgrabe and L. Meinel, “Tamper-proof tablets for distinction between counterfeit and originator drugs through PEG coding”, Eur. J. Pharm. Biopharm. 99, 1–6 (2016). https://doi.org/10.1016/j.ejpb.2015.11.009
- F. Tranchard, J. Gauthier, C. Hein, J. Lacombe, K. Brett, H. Villars, B. Sallerin, J.-L. Montastruc and F. Despas, “Drug identification by the patient: Perception of patients, physicians and pharmacists”, Therapies 74(6), 591–598 (2019). https://doi.org/10.1016/j.therap.2019.03.003
- Q.L. Her and S. Toh, “Sound-alike look-alike confusion and matching medication product attributes: simulated case-control studies”, Ann. Pharmacother. 53(10), 973–980 (2019). https://doi.org/10.1177/1060028019838239

Elsa Reallon
Elsa Reallon is a seventh grade of pharmacist student at the faculty of Pharmacy-University Claude Bernard Lyon-1, and a third grade of pharmaceutical resident in hospital pharmacist at Hospices Civils of Lyon, France. She is mainly involved in clinical pharmacy and takes a special interest in safety and quality management of hospital medication. 0000-0001-9201-2137
0000-0001-9201-2137
[email protected]

Anne-Laure Yailian
Anne-Laure Yailian is a hospital pharmacist at Hospices Civils of Lyon, France, in the hospital drug dispensation unit. She is particularly involved in the management of patients’ medication: from dispensing to patient information. She is strongly involved in the continuous improvement process of the unit (drug risk management, quality system). She was involved in the development and validation of the MIND database. 0000-0002-1399-1259
0000-0002-1399-1259
[email protected]

Chloé Marchand
Chloé Marchand is a hospital pharmacy resident at the end of the course and specialises in the preparation and quality control of hospital preparations. She will take up the position of assistant pharmacist specialist in charge of production within the Fripharm® unit of the Hospices Civils de Lyon, France.
[email protected]

Fabrice Pirot
Fabrice Pirot is professor in Pharmaceutical technologies and Biopharmacy at the Faculty of Pharmacy, University Claude Bernard Lyon-1, and hospital pharmacist at Hospices Civils of Lyon, France. He is the head of a hospital drug preparation and pharmaceutical control unit and Fabrication Research Innovation FRIPHARM university hospital platform. His research is focused on the development of drug delivery systems for the treatments of epithelial (e.g., nasal, ocular, bladder, oesophagus) diseases and disorders. 0000-0002-5750-4010
0000-0002-5750-4010
[email protected]