Johns Hopkins University engineers have used Raman spectroscopy and machine learning to understand the complex changes in tumours after immunotherapy. “Immunotherapy really works like magic and has fundamentally changed the way we view how cancer can be managed”, said Ishan Barman, a Johns Hopkins associate professor in mechanical engineering and a co-author of the study, which was conducted in collaboration with colleagues at the University of Arkansas. “However, only around 25 % of patients derive benefit from it, so there’s an urgent need to identify predictive biomarkers to determine who should receive the treatment.”
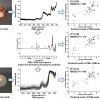
Using Raman spectroscopy, the team probed colon cancer tumours in mice treated with the two types of immune checkpoint inhibitors used in immunotherapy, as well as a control group of untreated mice. “This is the first study that shows the ability of this optical technique to identify early response or resistance to immunotherapy”, said Santosh Paidi, one of the lead authors who worked on the research as a mechanical engineering PhD student at Johns Hopkins. The method is also well-suited for exploring the compositional changes of the tumour microenvironment, rather than the cancer cells only.
“Rather than homing in on a few suspected molecules, we’re interested in getting a more holistic picture of the tumour microenvironment. That’s because the tumour is not just the malignant cell. The microenvironment contains a complex combination of the tumour stroma, blood vessels, infiltrating inflammatory cells and a variety of associated tissue cells”, said Barman. “Our idea is to take this approach and systematise it so it can be used by doctors to determine whether immunotherapy will be beneficial for the patient.”
The team used the Raman data with multivariate curve resolution-alternating least squares with support vector machine classifiers and random forests to train an algorithm to determine a range of features that were induced by immunotherapy.
“Our question was can we differentiate between the three groups, and then what are the specific spectral features that are allowing us to differentiate between them”, said Barman.
The team used data from different mice to build a machine learning classifier and test its performance. The goal was to mimic the biological variability the algorithm would encounter when presented with new data.
“You need to prove beyond a doubt that the differences that you’re seeing are immune checkpoint inhibitor-induced as opposed to just differences between two individuals”, said Barman. The results were promising, the team reported. “We were able to establish that collagen levels, lipid levels, and nucleic acid levels, as well as their spatial distribution in the tumour, change significantly when each immune checkpoint inhibitor therapy is given”, said Barman.
The differences were subtle but statistically significant and consistent with proteomics analysis conducted on the samples, pointing to the power of the technique for providing early signs of how a tumour is responding to treatment. More research is needed, but the team believes their work will pave the way to develop a method for predicting whether a patient will respond positively to immunotherapy.
“Combined with machine learning, Raman spectroscopy has the potential to transform clinical methods for predicting therapy response”, said Paidi.