Scientists at The University of Manchester have developed a technique which works by analysing compounds found in sebum—the oily substance that coats and protects the skin—and identifying changes in people with Parkinson’s Disease. Sebum is rich in lipid-like molecules and is one of the lesser-studied biological fluids in the diagnosis of the condition. People with Parkinson’s may produce more sebum than normal—a condition known as seborrhoea.
The work was sparked following an observation by Joy Milne, whose husband was diagnosed with Parkinson’s at the age of 45. Working with Dr Tilo Kunath at the University of Edinburgh, Joy demonstrated an incredible ability to distinguish a distinctive Parkinson’s odour in individuals using her sense of smell, even before symptoms emerge in those affected.
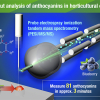
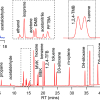
The team, led by Professor Perdita Barran, The University of Manchester, and the clinical lead Professor Monty Silverdale at Salford Royal Foundation Trust, recruited 500 people with and without Parkinson’s. Samples of sebum were taken from their upper backs for analysis. Using different mass spectrometry (MS) methods, 10 chemical compounds in sebum were identified which are elevated or reduced in people with Parkinson’s. This allows scientists to distinguish people with Parkinson’s with 85% accuracy.
The team confirmed their earlier findings that the volatile compounds on skin can be used to diagnose the condition, increasing the number of people sampled and including participants from the Netherlands, as well as the UK.
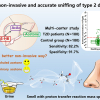
Now, with high-resolution MS they are able to profile the complex chemical signature in sebum of people with Parkinson’s and show subtle but fundamental changes as the condition progresses. Detailed analysis showed changes in people with Parkinson’s in lipid (fat) processing and mitochondria. Problems with mitochondria are one of the hallmarks of Parkinson’s.
This means this “world first” testing strategy is not only useful in diagnosing Parkinson’s but also in monitoring the development of the condition. The skin swab could provide an incredibly important new tool in clinical trials helping researchers measure whether new, experimental treatments are able to slow, stop or reverse the progression of Parkinson’s. The study unveiled novel diagnostic sebum-based biomarkers for Parkinson’s, provides insight into understanding of how the condition develops, and links lipid dysregulation to altered mitochondrial function.
These promising results published today could lead to a definitive test to diagnose Parkinson’s accurately, speedily and cost effectively. The team is now seeking funding to further develop the test, and explore the potential for using the test to “stratify” patients.
Working with the University of Manchester Innovation Factory, the team has patents filed for their diagnostic techniques and are planning to create a spin-out company to commercialise the new tests. They are also working to use this approach to develop tests for COVID-19 as shown in research published in EClinical Medicine as well as other conditions and are actively seeking investors interested in supporting the drive to bring this technology to market.
Professor Perdita Barran, Professor of Mass Spectrometry at The University of Manchester, said:
“We believe that our results are an extremely encouraging step towards tests that could be used to help diagnose and monitor Parkinson’s. Not only is the test quick, simple and painless but it should also be extremely cost-effective because it uses existing technology that is already widely available. We are now looking to take our findings forwards to refine the test to improve accuracy even further and to take steps towards making this a test that can be used in the NHS and to develop more precise diagnostics and better treatment for this debilitating condition.”
Parkinson’s tends to develop gradually and it may be many months, even years, before the symptoms become obvious enough for an individual to visit their GP. A DaTscan is regularly used to help specialists confirm the loss of dopamine-producing cells that cause the development of Parkinson’s. However, similar loss may also occur in some other rarer neurological conditions. With no molecular test for the condition, diagnosis is made by a neurologist based on a combination of symptoms such as tremor, slowness, stiffness and balance issues. However, many of the symptoms of Parkinson’s can overlap with other conditions, especially in the early stages when progression is gradual and symptoms are more subtle.
In a recent survey of more than 2000 people with Parkinson’s carried out by Parkinson’s UK, 26% reported they were misdiagnosed with a different condition before receiving the correct Parkinson’s diagnosis.
See ACS Central Science and Nature Communications.